In 2006 -- before I started blogging -- I had nine lovely months of pregnancy (Really. I didn't have complications, and I loved being pregnant. Both times, in fact.). Then we welcomed our first child into the world. I wish I would have journaled more of my thoughts and feelings at that time. Now that I am writing about her birth in detail, a little more than four years later, I can only do my best to remember.
I have always wanted to be a mom. I know I had small impressions, several times over a period of probably eight years, that my first baby would be a girl. During the pregnancy, I never felt that it was boy. (My husband and I checked the gender during the 19-week ultrasound anyway, and we were very excited to have a daughter. We had conceived her during his leave from Iraq, and this ultrasound was right after he returned home to stay.) We chose her first and middle name but, when talking to anyone else, we referred to her as "Top Secret," or "Topsy" for short, until after she was born. Later my husband began calling her "Shboogoo" -- the name I chose for my blog's URL.
****
Late on the night before my due date (which was actually 41 weeks, not 40, because my obstetrician changed the date after we had the ultrasound) , my contractions seemed to feel slightly different than the ones I had experienced during the previous week or so, but I didn't really know. Without telling my husband, I began writing down start times. We went to sleep looking forward to the next day: some friends were coming over for breakfast, and later in the day we would eat dinner with family.
At 4:00 a.m. on my due date I woke up and my contractions were more regular, coming every 15 minutes. Around 5:00 I woke my husband and told him what was happening. Later we called our friends to cancel the breakfast, but now I'm sure that we could have still done it.
Some time during our childbirth class my opinion -- that I would get an epidural if I needed it -- had changed. I
planned on a drug-free hospital birth with a
doula, and my husband was on board with that.
One of us called A., our doula, at 9:25 a.m. (according to her notes), to tell her my contractions were 12 minutes apart and 45-60 seconds long. She didn't need to come over yet, but it was nice to have her expertise over the phone.
Although it was cold, we walked outside, probably once around the condominium complex. A shower helped the contractions get closer together. I loved sitting on the birth ball. My husband was with me every second as I quietly breathed through contractions, and on his laptop he made a really cool spreadsheet with charts and graphs to track them. Nerd! By 3:20 p.m. they were 5 minutes apart and at least 80 seconds long, and at four I thought I felt a trickle of amniotic fluid releasing.
We asked our doula to come, with her counter-pressure and other doula skills. When she arrived I was on all fours. My contractions were spaced the same as a couple of hours earlier. She was impressed by my husband's spreadsheet; I don't think she had seen anyone do that before. Nerd! She was really helpful to me, which of course helped my husband, too.
My mom and two of my siblings came to visit, and brought leftovers from dinner. I remember eating a little four different times, and each time I threw up a while later.
After my husband took a nap we decided to go to the hospital, and we and the doula all got there around 9 p.m. (This was seventeen hours after labor began.) During the short drive there I actually told my husband I felt like I could be pretty dilated already. When the RN checked me I was 3 cm dilated and 90% effaced -- some progress since being at 2 cm two and a half days earlier. I don't know why they didn't send us back home, but it was probably because with the external fetal monitor they could see the baby's heart rate decelerating pretty low with each contraction. Apparently I was wrong about the trickle; I don't remember this, but the notes say, "waters are released." I guess that means the hospital staff talked to us about breaking my water for me, and we must have agreed to it.
We met (for the first time) the doctor who was on call. Because of the holiday weekend, the nurses' shifts were shorter, so the first one I had was off two hours after we arrived. Then it seemed that there was a new nurse every three or four hours (instead of every twelve)! I think the frequent changes and meeting new people slowed down my labor. By 11:20 p.m. the doctor wanted "change in an hour's time." I had the monitor on my belly again, and the baby's heart rate was still decelerating with each contraction, then returning to normal.
After midnight (Friday now) the new RN found that I was 3 cm or slightly more dilated, 95% effaced, and the baby was still at -1/-2 station. I ate flavored ice chips. We followed my doula's suggestions. However, the baby wasn't ready to come out. An hour later my contractions were 8 minutes apart. The nurse placed an I.V. in me. She started pitocin at 1 mL per hour, and we watched
Finding Nemo. She increased the pitocin about every half hour. The contrations were getting slightly closer -- and maybe more intense because that is one typical effect of pitocin -- but I think I felt fine.
The next RN checked me at 3:30 a.m.: 4 cm, 100% effaced, and +1 station. She turned off the pitocin at 4:15. Our baby's heart rate dropped into the 70s during contractions but she recovered well. The doctor came in and I was given antibiotics. At 5:30 I was still laboring without pitocin. I enjoyed slow dancing with my husband (
being vertical can let gravity help a baby descend). Unfortunately, my contractions were 8 minutes apart.
At 6:30 another new RN told me I was 4 to 5 cm dilated and +1 station. A new obstetrician came in a while later -- still not the one I had been seeing throughout my pregnancy, but I did think he was the friendliest of the three. The nurse placed an
internal fetal monitor and
IUPC to show more information than the external monitor gives. Almost an hour (not very long) after I had been checked, the OB checked me and in his opinion I was at 4 cm, 80% effaced and +1 station. He talked about the possibility that we would need a cesarean section to avoid infection because my membranes were ruptures. Twenty minutes late, they gave me pitocin again, followed by another IUPC (I think my movement from going over to the bathroom made this necessary), and
amnioinfusion to cushion the cord.
I had written in my birth plan that I preferred not to have these specific interventions. My labor was not how I had anticipated it, and in many ways you cannot plan a birth, since you do not know what problems might occur. Still, the interventions are more ridiculous to me now that I have done even more research on childbirth. Does it make sense to say that the baby needs to be
born within 24 hours of the water breaking or he/she is at risk of infection, but to do frequent vaginal exams (which
also increase the risk of infection)? By the way, if they broke my water the night before, it had only been 10 hours (not close to 24) and the doctor was already recommending a c-section.
My mom came at 8 a.m., partly to let my husband get some sleep. She's a wonderful mom. She felt bad that my labor was going on for so long (hers were only a few hours each). They gave me some oxygen. At 8:55, IUPC #3 was placed, and the pitocin increased to 2 mL per hour.
Around 9:15 the nurse was concerned about our baby's heart rate going down into the 60s; it was still recovering, though. She paged the doctor, stopped the pitocin, and
we decided to have a c-section because it seemed that the doctor thought it was necessary. It looked like the baby wasn't handling this very well and for some reason my cervix was not dilating. Also, we did not want her to have an infection, and I was tired and starting to get hungry since they only "allowed" me to have flavored ice chips.
They gave me
Terbutaline to "turn off" the contractions, and we waited for the doctor to return from delivering a baby at the other hospital. Meanwhile, they did the other (not fun) things to prep me for surgery. I was happy to know that we would definitely meet our baby within an hour. We had someone take our Wayne Egan CD into the operating room. The anesthesiologist walked to the operating room with me and my husband, and the
spinal anesthetic (which has a quicker onset than an epidural) and the entire surgery only took thirty minutes. I chose to have a curtain in front of me instead of watching. I'm sure my husband talked a lot to make me feel comfortable. The doctors liked having the relaxing piano music there (I did, too); I was their first patient to request that music play during a c-section.
I'm not sure if I wanted to smile.
Our daughter was born at 10:59 a.m. (This photo may gross some people out, but we like it. The hospital staff told us my husband could take pictures of the surgery.) We were more emotional than we thought we would be. We loved her immediately. She was beautiful!
The umbilical cord was long, and had been around her neck, shoulders, and waist, and tangled in her legs. Apparently that explained why her heart rate was dropping. She must have been grateful to be free of the cord squeezing her. Her
Apgar scores were good, though -- 7 and 9 -- so had she really been in distress? She weighed 6 pounds 3 and a half ounces, was 20 inches long, and had brown hair.
They reassembled my body and stapled the incision in my skin.
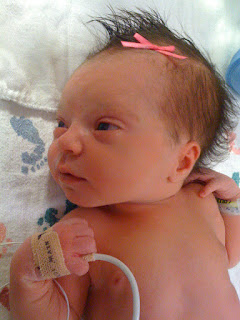
The first non-blurry photo of our first baby. She had a good cry!
First picture of our faces together; I couldn't hold her yet because of the anesthesia.
I wanted to see what was happening and longed to be part of it.
I remember the strangeness of having an operation (having done it
twice now makes it easy to remember): the cold room, shaking, feeling them touch and pull without causing me pain, and my arms being straight out away from my body.
After the doctors lifted my baby above the curtain to show me, and after my husband and I looked at each other when she first cried, I wondered when I would be able to have her near me. That picture of her and me above was just a short sweet moment. I know we went to our room at 11:30 and she was in the nursery (no, I don't know why) until 11:45. We are not sure when I first fed her. I think I slept most of that day. She didn't nurse correctly right away, but thankfully, we did figure out breastfeeding and continued for over thirteen months. She has been very healthy, and
she is one of our greatest blessings.
Held by daddy, having her first bath.
Family of three!
Nursed to sleep (probably her second or third day of life). This has always been my favorite baby picture of her, partly because it was my idea -- my husband took it from my perspective.
My doula for this birth, holding Shboogoo a few weeks after.